Epidural space is the space between the thecal sac and wall of spinal canal. It contains predominantly fat, also has venous plexus and connective tissue. It is best seen on MRI; more fat is seen posteriorly > anteriorly and in the dorso-lumbar > cervical spine. Normal contents include vessels and nerves, along with epidural fat. The CSF flow and the veins may give rise to artifacts, which must not be misinterpreted as a lesion.

Epidural fat appears as a sheet in the thoracic spine (A) and packets in the lumbar spine (B). Normal triangular shape (C) of the posterior epidural fat.
PATHOLOGIES
I] DEGENERATIVE: Often multi-level, with the most mobile segments most frequently affected; namely C1-C2, C5-C6, C6-C7, and L4-L5. Apart from the common presentations, atypical cases and sequelae of degenerative disc disease include:
a) Atypical disc degeneration: Young athlete, single level that may even calcify and worsen the stenosis.
b) Sequestered discs: These discs have a different signal intensity from the parent disc and may show peripheral enhancement on CE-MRI.

Signal intensity of sequestered discs (A & B) is often different from the parent disc. Peripheral enhancement on CE-MRI (C) helps in identifying sequestration.
c) Cystic degeneration of herniated discs.
d) Discal pseudocyst – Develops after microdisectomy. It actually represents post-operative seroma formation, and not a true disc.

Rare cystic degeneration (A & B) is best identified on fluid-sensitive images (A). Fluid accumulation after disc surgery such as microdiscectomy results in a discal pseudocyst (C & D).
f) Synovial Cyst – may cause spinal canal stenosis.

Spinal and lateral recess stenosis is often caused by synovial cysts. Detection is aided by fat suppression (A) and lack of central enhancement (C). L4-L5 is the commonest location.
g) Retro-odontoid cyst – can cause mass effect on cervico-medullary junction. Doesn’t show contrast enhancement.
h) Ossification of posterior longitudinal ligament – causes spinal canal stenosis. CT helps in confirmation as MRI may not demonstrate it accurately all the time. T2 hypointensity on MRI along the PLL may or may not represent calcification; hence perform a confirmatory CT in any MRI where you suspect OPLL.

Ossification of the Posterior Longitudinal Ligament (OPLL: A & B) usually results in spinal stenosis over multiple contiguous levels. Multilevel disk degeneration (C & D) can resemble OPLL on MRI (B vs D) and the diagnosis is thus best made on CT (A vs C).
i) Cystic degeneration of ligament flavum.

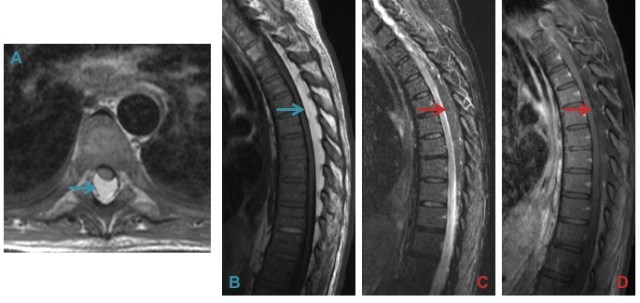
Cystic degeneration of the ligamentum flavum (A & B) is a rare cause of spinal canal and lateral recess stenosis. Sagittal images can be deceptive and spatial separation from the adjacent facet (solid arrow) allows differentiation from a synovial cyst.
II] INFECTIONS:
a) Spondylodiscitis – increased T2 signal intensity within disc space along with marrow edema.
b) Facet infection
c) Epidural TB
To differentiate between abscess (which usually requires surgery) and phlegmon (which may be managed with IV antibiotics), one needs to search for liquefaction in the center of the abscess on the post-contrast images with peripheral enhancement, compared to uniform enhancement in the latter.

Phelgmon (A & B) and Abscess (C & D) are differentiated based on the absence and presence of central liquefaction (solid arrow) respectively. While the management is based on neurologic status, an abscess often requires surgical decompression.
Epidural TB can present as a long segment serpentine lesion. Pure epidural TB without spinal involvement is rare but does certainly occur.
III] TRAUMATIC & VASCULAR: Hemorrhage is usually venous in origin.
a) Post-traumatic epidural hemorrhage
b) Spontaneous epidural hemorrhage – T1 hyperintense, hemosiderin rim and hyperdense on CT.

Post traumatic epidural hemorrhage (A & B) with C1-2 subluxation (solid arrow) and prevertebral edema (arrowhead). Post lumbar puncture hemorrhage (picture on extreme left) in the setting of acute leukemia and thrombocytopenia. Incidental paraspinal edema.
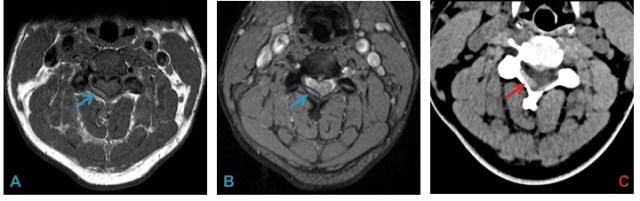
Relative T1 hyperintensity (A), hemosiderin rim (B) and hyperdensity on CT (C) aided in the diagnosis of epidural hemorrhage in this young patient. The cause of hemorrhage albeit, remained elusive after extensive work up.
c) Engorged venous plexus – can be seen in conditions like IVC thrombosis due to backpressure changes in the IVC. This can be easily diagnosed on CE-MRI as the midline anterior septum remains intact with enhancing venous structures seen on either side.

Backpressure from IVC thrombosis (A & C) causes congestion of the epidural venous plexus (A & B). Clue to the diagnosis is enhancement on each side of the midline septum (arrowhead).
d) Intracranial hypotension can also present as engorged venous plexus with diffuse pachymeningeal enhancement.

Epidural venous engorgement and dural thickening (A & B) from profound intracranial hypotension can often mimic a mass lesion. Clue to the diagnosis is diffuse pachymeningeal enhancement (C) seen on the brain MRI.
d) AV fistula/ AVM – show excessive flow voids on the MR images and can cause cord stenosis.
IV] Neoplastic
V] Others (the four F’s)
a) Fat – Epidural lipomatosis (suppresses on STIR)
Epidural lipomatosis is best depicted on T1 weighted images (A & B); the diagnosis is however based on signal loss on inversion recovery-fat suppressed sequences(C) and lack of enhancement on CE-MRI (D).
b) Flocculations – PNSTs or extramedullary hematopoeisis
c) Fluid – Arachnoid cyst (localized), CSF leak in cyst rupture.
d) Foreign Body – After Epidural catheter removal, granuloma formation may occur if a part gets broken off. Post kyphoplasty leakage may result in cement in the epidural space.
– Aneree Shah, DNB Radiology, Jupiter Hospital, Thane
– Akshay Baheti, Assistant Professor, Tata Memorial Hospital
– All images and legends courtesy Sumeet Dua, Assistant Professor, Rush University, Chicago