I. ARTHRITIS
Classification of arthritis:

Osteoarthritis
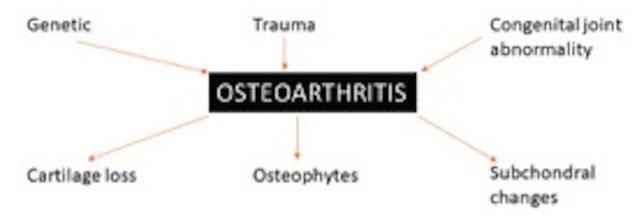
1. >80% of those aged above 50 years have osteoarthritis. It is multifactorial and has very variable appearances. It is the common end point of all kinds of arthritides.
2. Keep the report descriptive. Describe
a. Loss of joint space – how much and in which compartment?
b. Osteophytes- present or not
c. Subchondral cysts- present or not
3. While describing knee osteoarthritis, it is of utmost importance to describe about sparing of lateral femorotibial compartment as presence or absence of its involvement changes the management plan.
4. In the wrist, osteoarthritis most commonly involves the first metacarpophalangeal joint (trapezio-centric arthritis).
5. Scapholunate advanced collapse: combination of diminished radiocarpal joint space, scapholunate dissociation, and rotary subluxation of the scaphoid that allows the capitate to migrate proximally, produces SLAC. SLAC is the end stage of all wrist instabilities followed by radiocarpal OA.
Pathophysiology and radiologic correlation
1st: Articular cartilage destruction occurs first (initially picked on MRI) → Leads to narrowing of joint space (picked on x-ray) → May be asymmetric.
Complete cartilage loss may lead to a ‘bone on bone’ appearance, which indicates severe disease.
2nd: Subchondral cysts develop subsequently: The loss of cartilage leads to weakening of the subchondral bone and seepage of synovial fluid, which leads to the development of subchondral cystic changes.
3rd: Osteophyte formation happens subsequently.

Inflammatory arthiritis
Autoimmune condition. Rh factor negative arthropathies are calledseronegative spondyloarthropathies. HLA B27 is the next requested investigation.
Pathophysiology and radiologic correlation
1. These arthritides are characterized by marked thickening and inflammation of synovium with pannus formation. This has a tendency to involve ‘bare areas’ (which are not covered by articular cartilage) and between articular cartilage and capsule. The bare areas are the first site of inflammation as well as erosions. MRI catches these much earlier than X-rays.
2. Enthesis also seems to be target of damage.
3. Marginal erosions are seen due to proliferative pannus.
4. The earliest radiographic sign would be joint swelling and juxtaarticular osteopenia, due to inflammation and hyperemia with secondary bone resorption.
5. Joint subluxation may be seen.
6. Seronegative spondyloarthropathy often has spinal and SI joint involvement (less common in RA). Reiter’s syndrome (reactive arthritis) has a tendency to involve the midfoot joints.
7. Changes are initially reversible with biological therapy, and thus early detection is important before deformity and secondary OA sets in.
Differences between OA and inflammatory arthritis

Crystal arthritis
Crystals (monosodium urate in gout, and more commonly calcium pyrophosphate as in CPPD) are deposited inside and outside joint, which elicit a severe inflammatory reaction leading to arthritis. Unlike other arthritis, joint space is preserved till late in gout, as also bone density.
Key points to note while assessing plain film for arthritis
1. Soft tissues:
Presence of swelling indicates inflammatory arthropathy.
Calcifications may be seen in gout (chronic tophi) or CPPD (chondrocalcinosis/ pseudogout).
Soft tissue calcifications may also be seen in calcific tendinosis near a joint. In fact, the most common calcification is not monosodium urate in gout or pyrophosphate as in CPPD, but calcium hydroxyapatite as in calcific tendinosis.
2. Joint space
See whether joint space loss is symmetric or asymmetric. Remember that joint space and bone density are preserved till late in gout.
3. Subchondral and periarticular bone
Erosions may be seen in inflammatory arthritis while punched out erosions can be seen in gout. Subarticular cysts are seen in OA.
New bone (syndesmophytes) is seen in AS.
4. Alignment: Look for and describe loss of alignment, subluxation, and dislocation.

5. Joint distribution
Monoarthropathy is usually infective or crystal-related; may be OA.
Polyarthritis is seen in inflammatory arthiritis. Symmetrical involvement is more common in RA while asymmetric involvement is seen in seronegative arthiritis.
II. SPINE
Remember that relative ‘blind’ spots on spine MRI include the far lateral portion of the neural foramen, conus, presacral and prevertebral areas. Focus on them and don’t miss pathologies in these regions!
Disc pathology
1. Sagittal appearance of normal neural foramen is described as lambchop appearance
- Disc dessication: no loss of height, only dark signal
- Disc degeneration: loss of height + endplate changes
- Posterior annular fissuring: High signal on sagittal T2, report as ‘annular tear’ only when discogenic pain is present without other explanations for the pain on the scan. Otherwise it can also be described as a ‘high intensity zone’ if an incidental finding, a more agreeable term.
2. Abnormalities of disc contour include:
a. Depending on the pattern of disc herniation into the canal
Disc protrusion (AP< width), disc extrusion (AP>width), or Sequestered disc (separated from parent disc)



b. Depending on site of disc herniation:
Diffuse disc bulge
Central bulge or paracentral bulge: central and paracentral account for ~90% of cases
Foraminal: ~4-5% of cases, easy to identify on sagittal
Extra-foraminal/far lateral: ~4-5% of cases, easy to identify on sagittal
III. MISCELLANEOUS POINTS
1. Synovial cysts
These are well defined, usually at L4-5 level, seen on the margins of sagittal sections, usually T1 dark and T2 bright (can be T1 bright due to hemorrhage/protein), and can lead to central stenosis. Treatment is via needle access to cyst and aspirate/inject steroid.
2. Spinal canal stenosis
Can be central/lateral/foraminal. Causes include degenerative (facet arthropathy, ligamentum flavum, disc bulge), spondylolisthesis, facet cysts, congenital short pedicles, and tumor. amongst others.
Central stenosis:
The degree of thecal sac compression should be commented upon: severe (no CSF)/ moderate (some CSF present)/ mild (good amount of CSF present). In severe stenosis, cauda equine will appear buckled.
Lateral recess stenosis:
Note that the lateral recess is present at the medial aspect of the pedicles, while the neural foramen is lateral to the pedicles. Nerve roots lie in the recess after leaving the thecal sac, and then exit via the neural foramina
Lateral recess stenosis usually occurs due to hypertrophic facet joints or degenerated discs, and leads to compression of the nerve below disc level
3. Post operative imaging/Epidural fibrosis
Patients may develop recurrent back pain despite surgery. MRI is then needed to differentiate between recurrent disc (which won’t enhance) (failed back syndrome) vs scar tissue (enhances). Thus, one must give contrast in recurrent back pain in the post-operative setting.
4. Marrow abnormalities
T1WI usually more useful than T2WI.
Osteoporotic fracture will have an otherwise normal to bright signal on T1WI.
Pathological fracture will have abnormal replaced marrow, well appreciated on T1WI as T1 hypointense foci. Posterior elements and paravertebral areas will be often involved.
5. Arachnoiditis
Causes: spinal surgery, infection etc
Empty sac sign: Nerve roots get stuck to dura, so the thecal sac appears empty on axial images
– Somesh Singh, Senior registrar, Tata Memorial Hospital
– Sureshkumar Gudi, Senior registrar, Tata Memorial Hospital
– Nikshita Jain, Senior registrar, Tata Memorial Hospital
– Siddharth Thaker, Innovision Imaging

Arthritis simplified!
LikeLike